ADMIN
(0 comments, 229 posts)
This user hasn't shared any profile information
Posts by ADMIN
Better Model Used to Further Development of HIV Vaccine
One of the best ways to stop the spread of disease is through vaccines. This long-used defense has halted numerous and dangerous infections over the years. It is no wonder then that scientists are urgently searching for ways to develop an HIV vaccine. A number of factors present obstacles that have, so far, stood in the way of progress.
3 Struggles in the Search for a HIV Vaccine
The menacing virus is an elusive microbe that evades detection both from the human immune system and most HIV vaccine models tested against it. What makes the virus so effective is the ability it has to mutate, which happen rapidly. Vaccines generally work by using non-infectious material and introducing it into the body where the immune system can identify and then attack it. The quickly changing virus means that a lesser amount of the virus is actually found and eliminated.
Another factor that gets in the way is the design of the HIV itself. The virus is packed into a type of envelope, which is coated with sugars that come from the host. Because this is on the outside of the microbe, it makes it difficult for the immune cells to identify it as an intruder.
A third issue in the mix is the lack of a living model that researchers can use to test potential HIV vaccines. This last obstacle has limited progress the most. Recent developments may finally change that.
A team of researchers has found that a certain species of primates has an immune system that closely resembles that of the human immune system. In order to be able to use this to their advantage, a virus that resembled HIV but that could infect the animal, had to be developed. The researchers, with some trial and error, were able to accomplish this. The result is a virus that infects and creates AIDS-like symptoms in the host animal. With a better model to test vaccines and monitor the viral envelope, they are hopeful to speed up HIV vaccine research and development.
Enlightening Effect of Observing HIV Cellular Transmission
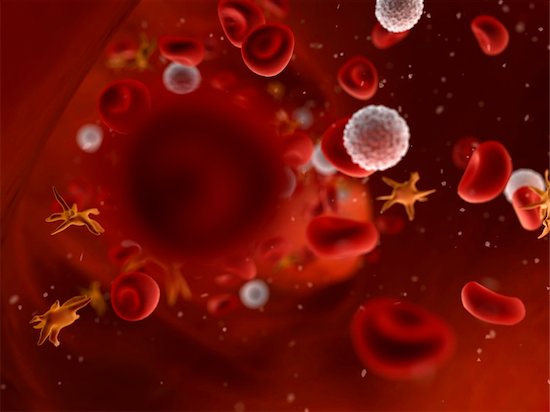
Scientists have discovered some interesting facts about the cellular transmission of HIV and how the virus moves throughout the body.
The inner workings of HIV, and the effectiveness with which it is able to transmit and spread infection, are complex. HIV cellular transmission has been carefully studied now for decades. The virus establishes itself in the host a couple of ways, and new information continues to be discovered. Cell-to-cell transmission has also been observed in the lab. Scientists have now been able to track HIV as it infects cells in real time in living organisms. This has big implications for the current approach to treatment and therapy.
Immune Cellular Transmission and the Role of Mutation
In this latest study, tracking HIV cellular transmission from cell to cell revealed a number of facts. First, the infected immune cell meets up with an uninfected cell, both being CD4 helper T cells. A sort of bridge is constructed between the two, and viral material that is passed along infects the second cell. The process, according to the researchers, is similar to the way nerve cells communicate information with each other. Cellular transmission works quickly. Several copies of the virus can pass through the bridge, making mutation easier. Mutant forms of the virus make it easy to escape detection from the immune system. This potent means of infection could prompt researchers to look to new approaches for treatment. Cell-to-cell transmission may increase resistance to antibodies, and the cells seem more resistant to current treatment options.
Today, antiretroviral therapies target viral particles floating in the bloodstream. It could be that cell-to-cell transmission takes place rapidly and goes undetected until the virus can be found in the blood. Reservoirs of infected cells are found in different tissues. Once infected, the immune cells can replicate, and clusters form rapidly. Treatments focusing on limiting or halting cell-to-cell transmission may be more effective at curbing the infection than current methods. Evidence that this could be useful if applied to potential vaccines was indicated as well.
In the U.S. alone, over one million people are living with HIV, and almost 40 million cases worldwide, so the search for effective treatments continues.

HIV DNA Successfully Removed from a Living Cell
HIV treatments have dramatically improved in recent years. Combinations of antiretroviral medications target the replicating of HIV within the body. When taken regularly, many HIV-positive individuals can lead relatively normal and healthy lives. As beneficial as these treatments are, researchers are still looking into finding an actual cure for the disease. One reason: if treatment happens to be interrupted, the virus quickly makes a comeback, and the infection can progress to AIDS. This is due to the latent HIV DNA within the cells.
Without the medications to suppress the virus, the infected cells are free to reproduce. Removing these viral pieces from the infected cells, and other areas where they lay dormant, is what would eradicate the infection.
HIV DNA: Gene Editing Takes the Next Step
In line with this objective, one recent study has successfully removed the HIV DNA from infected cells. The team had developed a sort of gene editor. The system works by targeting the infected cells and removing specific segments of HIV’s genetic material implanted by the virus.
When first tested, results were positive, and had little-to-no adverse effects. The most recent trial included targeting HIV material in organ tissue and blood cells. After just a couple of weeks, every type of tissue showed signs of the viral genetic material being removed. The broad spectrum of tissues gives hope that further developments will yield lasting and effective results, especially if gene editing is used in conjunction with current therapies.
Researchers are confident that if used alone, it has the potential to eliminate HIV from the body. Added benefits may come from using it along with antiretroviral therapies. Suppressing the virus’ ability to replicate, and removing its DNA from infected cells (even latent ones), will ensure a clean sweep. Seeing as the gene editing is also a very flexible technique, it is possible to tailor it to target mutated forms of the virus—an issue that continues to impede progress.
While the results from this study have years of trials and testing to go, it shows that medical objectives in regard to HIV and HIV DNA are feasible.

The Enzyme That Could Be Used Against HIV
HIV can now be managed as a chronic disease, largely due to modern antiviral medications. These medications target the enzyme, protease. Inhibiting the enzyme aids in preventing the infection from spreading within the body by slowing the maturing process. However, studies are now showing that the very enzyme that speeds up maturation can also destroy the virus if certain processes were to be delayed. This could mean that within a decade we will see a new generation of medications used to treat and manage HIV with potentially fewer side effects.
Halting the Spread by Activating the Enzyme Early
Once a cell is infected, a sort of bud forms from the cell. This sac-like structure contains viral particles that will soon become mature HIV. Once the bud is released, it is the protease enzyme that goes to work in order to morph the particles into a mature, infectious virus. Afterward, it floats around until a new, healthy cell is found and infected, thus starting the process over again. This then makes it understandable why the current therapies are aimed at stopping protease. Researchers have found, however, there are certain factors that, when changed, can cause the enzyme to activate prematurely. If this happens prior to the bud releasing from the host cell, it means the viral particles that were released will not be able to mature, and thus are not infectious.
When the protease activates before the bud releases, it causes a leak of proteins and enzymes into the host cell. Once the bud actually releases, there is no more enzyme to trigger the maturing phase. How does protease activate early? Everything works on the precise timing of events. The viral interaction with certain proteins is important to timing the release. Should an interaction be compromised, a delay can occur. The protease activates regardless of whether the bud has separated or not. With the release time delayed and the proteins gone, there is nothing left for the virus when the bud is finally detached, and it is rendered impotent.
Current medications can cause a spectrum of side effects that are often experienced. Therefore, many programs and studies are focusing on effective therapies with fewer side effects.
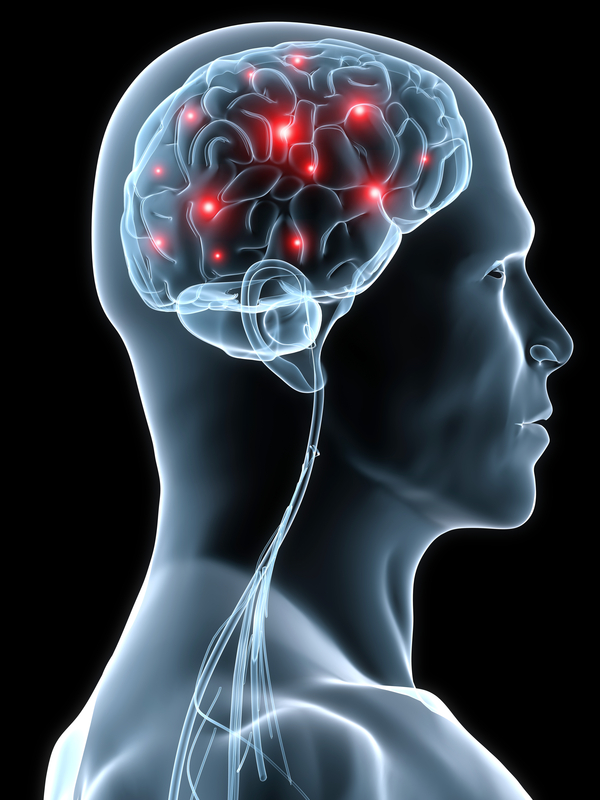
Neurological Issues May Be Among HIV’s First Symptoms
Neurological issues have been noted in patients who had recently been infected with HIV. There are a host of conditions that are associated with HIV infection and disease progression. Most treating physicians are aware of many of these and keep a close eye on their HIV-positive patients. However, it was recently noted that as early as just a few days after the infection, certain symptoms and issues can present in patients not yet diagnosed or treated for HIV infection. Many have been diagnosed with HIV after presenting with neurological symptoms.
A Study Reveals How Common Neurological Issues Are
In a recent study, a group of individuals was followed to find out more about early HIV infection and its effect on the nervous system. Participants all had recently been infected. For some, it had been only a few days, and for others, it was up to two months since the time of infection. Out of those followed, over half presented with neurological issues, including neuropathy (disease of the nervous system), cognitive trouble, and motor difficulties. In many instances, patients had experienced more than one type of the mentioned issues. In rare instances the conditions were severe.
The Benefits of Treatment in Reducing Neurological Symptoms
Such early stages of infection are generally undetectable by standard HIV testing as the immune response has yet to build. Neurological symptoms were noticed before any others in most cases. Once antiretroviral therapies were started, 90% of the neurological issues were resolved. For some, lingering symptoms were observed even after months of treatment. When researchers compared the lab tests, those with persistent symptoms also had higher viral levels in the blood. These findings show that the virus has a profound effect on the nervous system. The good news, however, is that most of the conditions cleared up with treatment.
Study on the subject is ongoing. Other issues as well are brought to light. For example, in the development of new treatments against HIV, researchers are considering taking into account the role of the brain and nervous system. Some theorize that latent HIV could be lurking in these areas, therefore causing issues early on. So new questions are raised, and delving further into the topic continues.